What Is Minimally Invasive Spine Surgery?
Minimally invasive spine surgery refers to a group of procedures designed to treat structural problems in the spine through smaller access points and more targeted techniques.
Rather than opening a large section of the back and moving muscle aside for the duration of surgery, these procedures use specialized instruments that pass through or between muscle layers. This allows the surgeon to reach the affected area with less disruption to surrounding tissue.
These techniques are commonly used to address conditions involving disc damage, nerve compression, or instability within the spine. In many cases, they achieve the same goal as traditional surgery, but with a different approach to how the spine is accessed.
The benefit is not simply smaller incisions. It is a more focused way of treating the problem.
When Is Minimally Invasive Spine Surgery Considered?
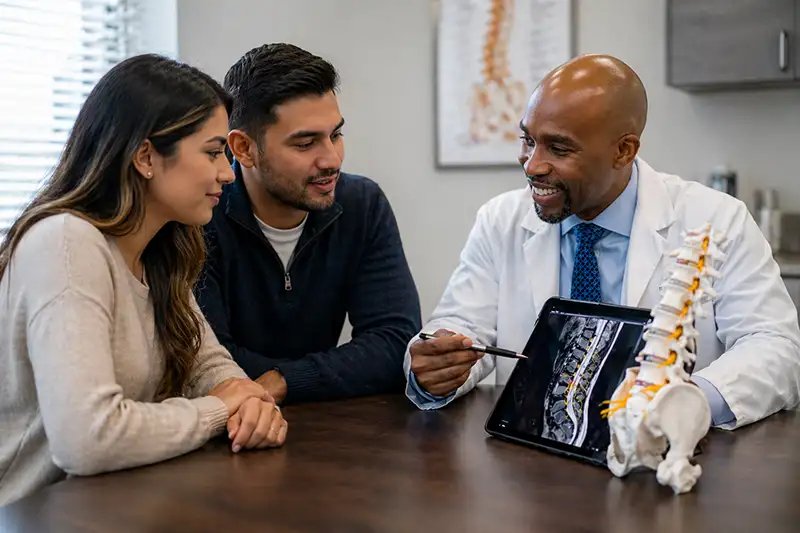
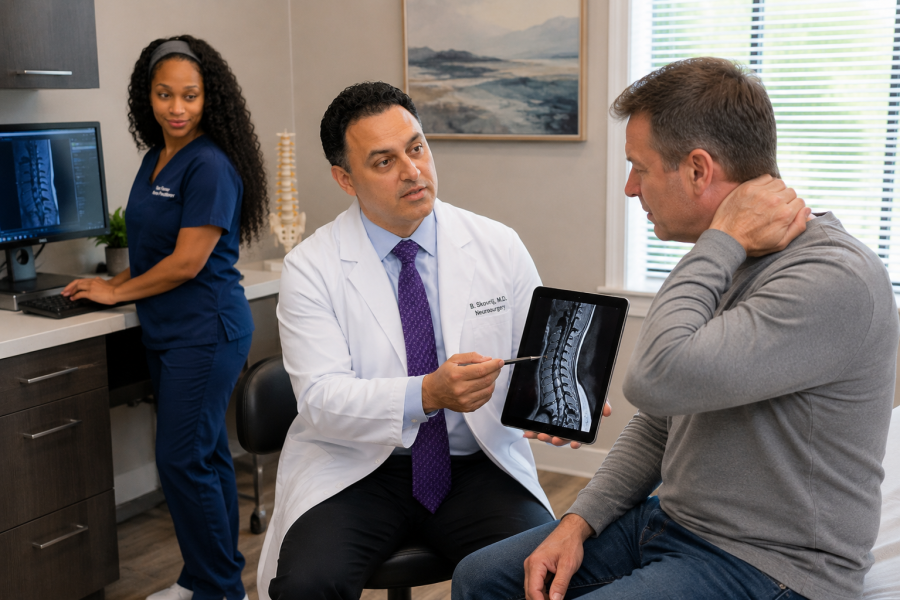
Surgery is not the starting point. It is considered when a clear structural issue is present and other treatments have not provided enough relief.
This typically includes situations where:
- Pain continues despite physical therapy, medication, or injections
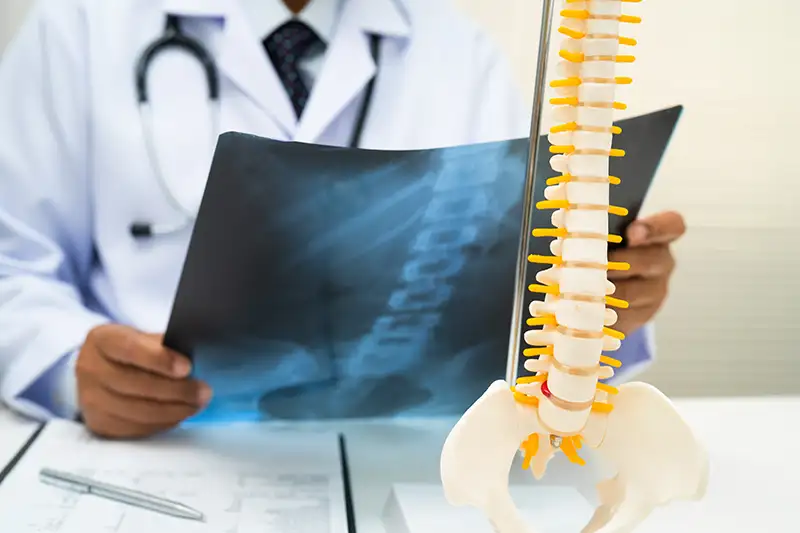
- Imaging shows disc damage, instability, or nerve compression
- Symptoms are affecting strength, mobility, or daily function
- Nerve-related symptoms such as numbness or weakness are progressing
In many cases, patients have already gone through multiple stages of treatment before reaching this point.
The decision to move forward is based on alignment between symptoms, imaging, and prior response to care.
How Minimally Invasive Spine Surgery Is Performed
Minimally invasive procedures are performed using imaging guidance and specialized instruments designed for precision.
Through small incisions, the surgeon is able to:
- Access the affected spinal level
- Remove material that is compressing a nerve
- Stabilize the spine when necessary
Real-time imaging is used throughout the procedure to guide placement and confirm accuracy.
The exact approach depends on the condition being treated. Some procedures focus on relieving nerve pressure, while others address instability within the spine.
Each step is designed to correct the underlying issue while limiting unnecessary disruption to surrounding structures.
What To Expect After Minimally Invasive Spine Surgery
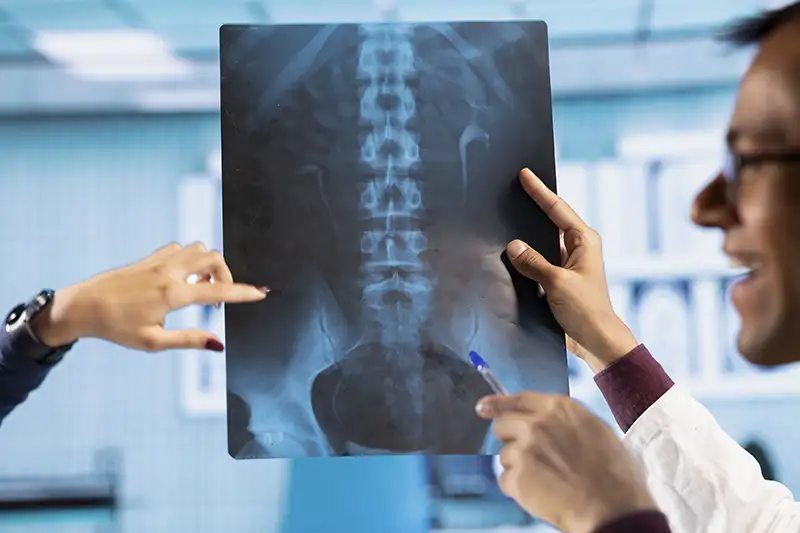
Recovery varies depending on the procedure and the condition being treated, but the general pattern is more gradual than immediate.
Many patients are able to:
- Begin moving shortly after surgery
- Return home the same day or after a short stay
- Resume light activity within a few weeks
Some soreness and temporary nerve symptoms can occur early in recovery as the body adjusts.
Over time, improvement tends to follow the same path as the original symptoms, gradually decreasing as pressure is relieved and function returns.
Full recovery depends on healing, activity level, and the extent of the original condition.
Frequently Asked Questions About Minimally Invasive Spine Surgery
How is minimally invasive surgery different from traditional spine surgery?
The difference is in how the spine is accessed. Minimally invasive techniques use smaller incisions and targeted instruments, which can reduce tissue disruption and recovery time compared to traditional open procedures.
Am I a candidate for minimally invasive spine surgery?
That depends on your diagnosis, imaging findings, and how your symptoms have responded to treatment. Some conditions are well suited for minimally invasive approaches, while others require a different strategy.
How long does recovery take?
Recovery varies by procedure. Some patients return to light activity within weeks, while others require a longer period depending on the complexity of the condition.
Will I need spinal fusion?
Not always. Fusion is considered when instability is present. Other procedures may focus only on relieving nerve compression.
Is surgery the only option at this stage?
Not necessarily. Surgery is considered when other approaches have not worked and the cause is clearly defined. The goal is to match the treatment to the condition, not move too quickly into surgery.
What happens if I wait too long?
In some cases, delaying treatment can allow nerve compression to worsen. When weakness or loss of function develops, timing becomes more important.