What Is Spinal Stenosis?
Spinal stenosis refers to a narrowing of the space within the spine where the spinal cord and nerves travel. That narrowing does not always cause symptoms on its own. It becomes a clinical problem when the available space is reduced enough to place pressure on the nerves, disrupting how signals move between the spine and the rest of the body.
Spinal canal narrowing most often affects the lower back and neck, where the spine absorbs the most mechanical demand. In lumbar spinal stenosis, the narrowing occurs in the lower back and frequently affects how the legs function during activity. In cervical spinal stenosis, the narrowing occurs in the neck and can affect the arms, hands, and even walking stability.
Unlike an acute injury, spinal stenosis usually develops over years. Many patients adjust gradually without fully recognizing what is changing until walking, standing, or simple daily movement becomes noticeably more difficult.
What Causes Spinal Stenosis?
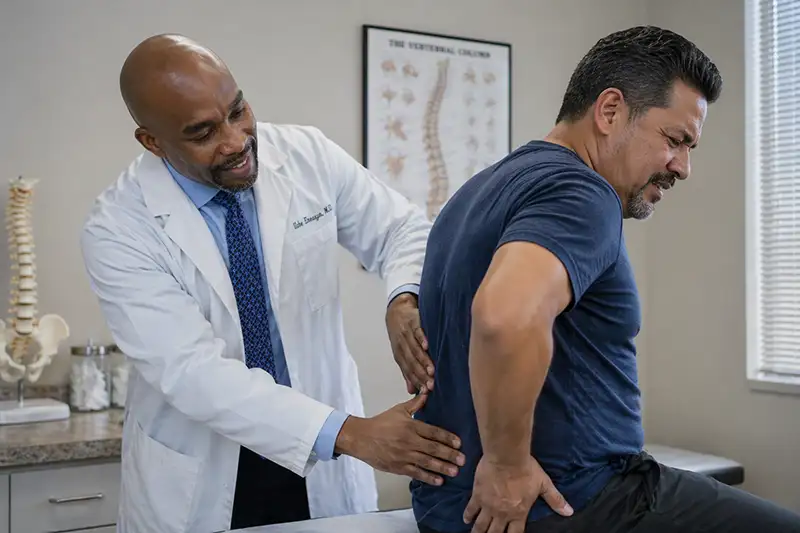
Spinal stenosis is rarely caused by a single issue. It typically develops as several structural changes occur together, each contributing to reduced space within the spinal canal. Understanding the cause helps determine which approach to spinal stenosis treatment makes the most sense for each patient.
Common contributors include:
- Degenerative disc changes, where discs lose height and alter spacing between vertebrae, allowing bones to shift closer together
- Bone spur formation, which can grow into the canal and compress nearby nerve tissue
- Thickening of spinal ligaments, especially the ligamentum flavum, which can fold inward and reduce available space
- Disc bulging or herniation, which may press directly against the spinal cord or exiting nerve roots
- Spinal instability or spondylolisthesis, where vertebral slippage changes alignment and narrows the canal further
- Facet joint arthritis, which contributes to joint enlargement and additional compression
These changes often develop slowly over years. In many cases, symptoms become apparent only after the space has narrowed beyond a certain threshold, which is why a structured evaluation is important when activity limitations begin.
Symptoms of Spinal Stenosis
Symptoms depend on where the narrowing occurs and how severely the nerves are affected. Because the condition progresses gradually, many patients notice changes in their activity tolerance well before they associate those changes with a spinal problem.
In the lower back, patients with lumbar spinal stenosis often describe:
- Pain, heaviness, or cramping in the legs when walking or standing for extended periods
- Symptoms that ease when sitting down, bending forward, or leaning on a shopping cart
- A gradual reduction in how far they can walk before needing to stop
- Numbness or tingling that affects one or both legs
- Weakness in the legs that develops with activity
In the neck, cervical spinal stenosis symptoms may include:
- Stiffness or aching that extends into the shoulders or upper back
- Numbness, tingling, or weakness in the arms or hands
- Reduced grip strength or difficulty with fine motor tasks
- Changes in walking balance or a sense of unsteadiness
- In more advanced cases, changes in bladder or bowel control that require prompt evaluation
These patterns tend to develop slowly. Many patients modify their routines over time without connecting those changes to nerve compression in the spine. When those limitations begin to affect daily life, an evaluation helps identify the source.
Spinal Stenosis Treatment in NJ
Treatment is determined by how much the narrowing is affecting nerve function, how long symptoms have been present, and how the patient has responded to previous care. Most patients with spinal stenosis begin with conservative options and move toward more targeted approaches if symptoms persist or progress.
Early and Non-Surgical Care
- Activity modification to reduce strain during walking or prolonged standing
- Physical therapy focused on flexion-based positioning, posture, and spinal support
- Anti-inflammatory medication to manage acute flare-ups
- Structured monitoring to track how symptoms respond over time
Interventional Pain Management
For patients whose symptoms are not controlled with conservative care, targeted procedures can reduce inflammation around compressed nerves and improve daily function:
- Epidural steroid injections, used to deliver anti-inflammatory medication directly around affected nerve roots
- Facet joint injections, when joint-related changes are contributing to canal narrowing
- Radiofrequency ablation, when facet-mediated pain has been confirmed through diagnostic injections
These approaches are frequently used to reduce symptoms, restore activity tolerance, and gather information about which structures are most involved.
Targeted Procedures for Stenosis
When specific structural contributors are identified, more focused interventions may be appropriate:
- The MILD procedure, used when thickened ligamentum flavum tissue is a primary driver of narrowing
- Disc-focused procedures, when disc changes are playing a central role in nerve compression
When Symptoms Continue
If symptoms persist despite conservative and interventional care, or if imaging suggests more significant nerve compression, evaluation moves to the next level:
- Advanced MRI review to assess the extent of canal narrowing and level of involvement
- Consultation with a spine specialist to discuss surgical candidacy
- Surgical intervention, considered when walking ability, strength, or daily function are clearly affected and other approaches have not provided adequate relief
For most patients, the goal is to restore function with the least invasive approach that produces durable results. A full evaluation helps determine where to begin.
Frequently Asked Questions About Spinal Stenosis
How do I know if my symptoms are from spinal stenosis?
The pattern is often the clearest indicator. Symptoms that build with walking or standing and improve with sitting or leaning forward are commonly associated with lumbar spinal stenosis. A full clinical evaluation, including imaging review, confirms whether that pattern is originating from the spine and how much canal narrowing is present.
Does spinal stenosis get worse over time?
It can. Because the condition is tied to structural changes in the spine, it may continue to progress gradually if left unaddressed. Some patients remain relatively stable over time, while others notice increasing limitations with activity. Regular monitoring and timely treatment help manage this progression.
Is spinal stenosis the same as a herniated disc?
No, though the two can occur together. A herniated disc involves disc material pressing on a nerve root. Spinal stenosis refers to a broader narrowing of the spinal canal itself, which can affect multiple nerve roots. Both conditions involve nerve compression in the spine, and both are evaluated through imaging and clinical examination.
Will I need surgery for spinal stenosis treatment in NJ?
Most patients begin with non-surgical options, and many find meaningful relief without surgery. Surgical evaluation is considered when symptoms significantly limit mobility, when nerve compression continues despite other care, or when imaging confirms a level of narrowing that is unlikely to respond to conservative treatment.
Why does walking make symptoms worse?
Walking places the spine in a more extended position, which can further narrow the canal and increase pressure on the nerves. Sitting or bending forward opens up space within the canal, which is why many patients find relief in those positions. This pattern, sometimes called neurogenic claudication, is one of the more recognizable signs of lumbar spinal stenosis.
Can spinal stenosis affect both legs?
Yes. Because spinal stenosis involves narrowing of the central canal rather than compression of a single nerve root, both legs are often affected. This bilateral presentation is one of the features that distinguishes spinal stenosis from a disc herniation, which more commonly affects one side.
What makes a patient a candidate for the MILD procedure?
The MILD procedure is typically considered when thickened ligamentum flavum tissue is identified as a primary contributor to canal narrowing. It is a minimally invasive outpatient procedure that removes excess ligament tissue to restore space within the canal. Candidacy is determined through imaging review and clinical evaluation.