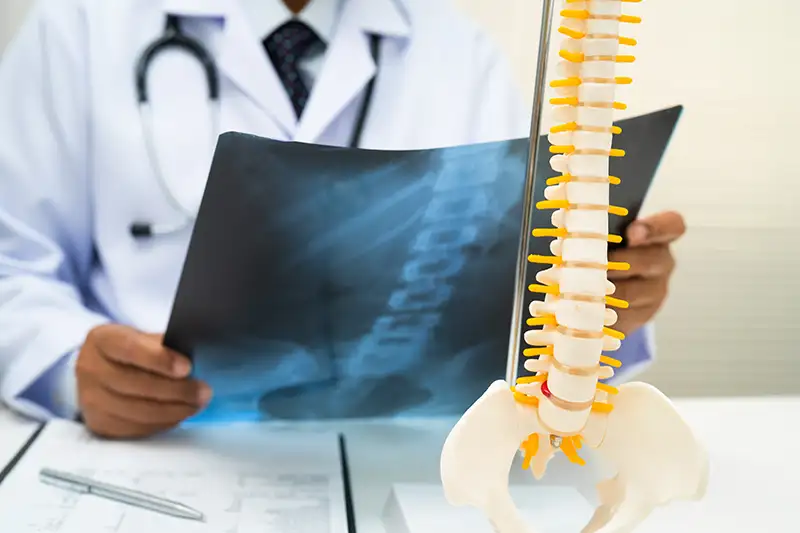
What Causes a Herniated Disc?
A herniated disc rarely comes from a single moment. More often, it develops over time and becomes noticeable when the disc reaches a point where it can no longer handle normal stress.
Common contributing factors include:
- Gradual disc degeneration, where the disc loses flexibility and becomes more prone to tearing
- Repeated strain, often from lifting, twisting, or prolonged sitting
- Sudden force or injury, such as a fall or motor vehicle accident
- Postural habits, especially when the spine is under constant uneven pressure
- Increased load on the spine, which can accelerate wear on the discs
In many cases, the event that triggers pain is not the true cause. It is simply the point where the underlying issue becomes noticeable.
What Causes a Herniated Disc?

A herniated disc rarely comes from a single moment. More often, it develops over time and becomes noticeable when the disc reaches a point where it can no longer handle normal stress.
Common contributing factors include:
- Gradual disc degeneration, where the disc loses flexibility and becomes more prone to tearing
- Repeated strain, often from lifting, twisting, or prolonged sitting
- Sudden force or injury, such as a fall or motor vehicle accident
- Postural habits, especially when the spine is under constant uneven pressure
- Increased load on the spine, which can accelerate wear on the discs
In many cases, the event that triggers pain is not the true cause. It is simply the point where the underlying issue becomes noticeable.
Symptoms of a Herniated Disc
Symptoms vary depending on where the disc is located and whether a nerve is involved.
Common patterns include:
- Pain that begins in the neck or lower back and extends outward
- Discomfort that worsens with sitting, bending, or certain movements
- Stiffness that limits normal range of motion
- When a nerve is affected, symptoms often change:
- Pain that travels into the arm or down the leg
- Tingling or numbness along a specific path
- A burning or electric sensation
- Weakness in the arm, hand, leg, or foot
These patterns are not random. They often follow the path of the affected nerve, which helps identify the source of the problem.
Treatment Options for a Herniated Disc
Treatment depends on how the disc is affecting surrounding structures and how symptoms have responded to prior care.
That may include:
Early and Non-Surgical Care
- Physical therapy focused on movement and stability
- Anti-inflammatory medications to reduce irritation
Interventional Pain Management
- Epidural steroid injections to reduce nerve inflammation
- Targeted injections to confirm and treat the source of pain
Further Evaluation
- Imaging such as MRI to assess disc and nerve involvement
- Review of how symptoms respond to targeted treatment
When Symptoms Continue
- More advanced spine evaluation
- Consideration of surgical options when a structural issue is clearly defined
Surgery is not the starting point. It is considered when symptoms persist, imaging confirms the cause, and other approaches have not provided relief.
Frequently Asked Questions About Herniated Discs
What is the difference between a herniated disc and a bulging disc?
A bulging disc extends outward but remains intact. A herniated disc involves a tear, where inner material pushes through and may contact a nerve.
Can a herniated disc heal on its own?
Some cases improve over time, especially when symptoms are mild. Persistent or worsening symptoms often require evaluation to determine the cause.
When should I seek evaluation for a herniated disc?
If pain continues, spreads into the arms or legs, or includes numbness or weakness, it’s worth a closer look.
Will I need surgery?
Most patients do not. Surgery is considered only when symptoms persist and imaging confirms a structural issue.
What makes symptoms worse?
Sitting for long periods, bending forward, lifting improperly, or movements that increase pressure on the spine can aggravate symptoms.