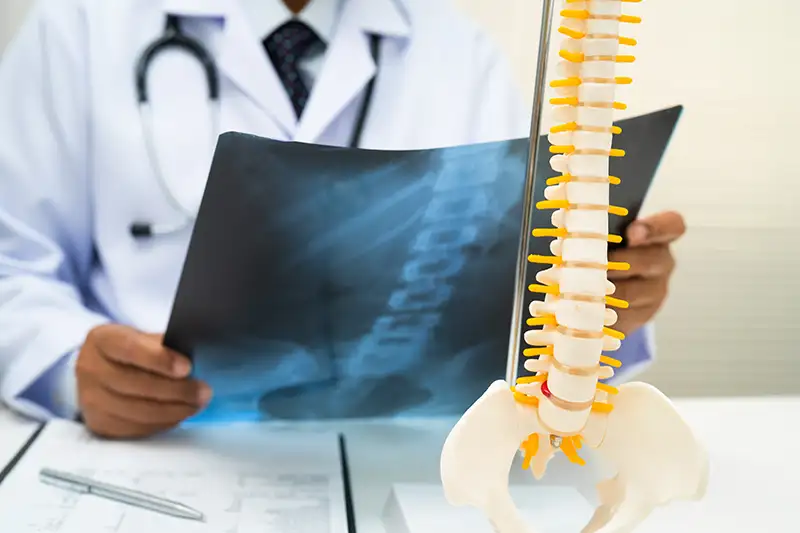
What Is Sciatica & Radiculopathy?
Radiculopathy is the clinical term for nerve root dysfunction caused by compression or irritation where a nerve exits the spinal column. Sciatica is the most recognized form. It develops specifically when the sciatic nerve, which originates in the lower lumbar and sacral spine and runs through the buttock and down the leg, is placed under pressure.
Both conditions are diagnosed based on symptom pattern, physical examination, and imaging. A nerve root that is compressed may produce pain, numbness, tingling, or weakness, and in many cases, all of these at once.
What Causes Sciatica & Radiculopathy?

Radiculopathy develops when something reduces the available space around a nerve root, either at the point where it exits the spine or within the spinal canal itself. The cause determines the best course of sciatica treatment, which is why evaluation focuses on identifying the specific structural issue before any treatment decision is made.
Common structural causes include:
- Disc herniation or bulging, where disc material pushes outward and presses against a nearby nerve root. This is the most frequent cause of both sciatica and lumbar radiculopathy, particularly in patients under 50.
- Degenerative disc disease, where the disc loses height and the vertebrae shift closer together, narrowing the openings through which nerve roots exit.
- Spinal stenosis, where the spinal canal or nerve exit points become narrowed due to bone changes, ligament thickening, or a combination of structural changes.
- Bone spur formation, where overgrowth of bone around degenerating joints or discs gradually encroaches on nerve tissue.
- Spondylolisthesis, where forward slippage of one vertebra over another can pinch the nerve root traveling near that level.
- Facet joint inflammation, where acute or repetitive strain causes inflammation around the nerve root, producing radiculopathy without direct structural compression.
- Piriformis syndrome, which applies external pressure to the sciatic nerve through the muscle rather than at the spinal level. This is less common but is sometimes confused with true lumbar radiculopathy.
In some patients, more than one of these factors is present simultaneously. A herniated disc at one level may exist alongside mild stenosis at another, with the combined effect placing enough pressure on the nerve to produce symptoms. This is why imaging review and clinical evaluation go together rather than in sequence.
Symptoms of Sciatica & Radiculopathy
Radiculopathy does not behave the way most musculoskeletal pain does. It follows a nerve pathway, which is why it often feels unrelated to the spine even when the spine is entirely responsible. Understanding this pattern is one of the first steps in connecting symptoms to a diagnosis.
Lumbar Radiculopathy and Sciatica
When the nerve root involved is in the lower back, patients typically notice:
- Sharp, shooting, or burning pain that travels from the lower back or buttock into the leg, sometimes reaching the calf or foot
- Numbness or tingling along a specific band on the outer thigh, calf, or top of the foot
- Weakness in the leg or foot, sometimes described as difficulty lifting the front of the foot while walking
- Pain that worsens when sitting for long periods, coughing, sneezing, or straining
- A sensation that feels like pins and needles or electric shocks rather than a dull ache
- Symptoms typically affecting one side, though bilateral involvement is possible when the central canal is narrowed
Cervical Radiculopathy
When compression occurs in the neck, symptoms follow the affected nerve into the arm rather than the leg:
- Pain that begins in the neck and travels through the shoulder, upper arm, or into the hand
- Numbness or tingling in the fingers or specific parts of the hand, depending on which level is involved
- Weakness in the grip or shoulder muscles
- Difficulty with fine motor tasks such as buttoning clothing or holding objects
- A deep aching sensation in the shoulder blade area that does not respond to shoulder-focused treatment
Because these symptoms often develop gradually, many patients adapt their daily routine before they connect the discomfort to a nerve issue. Sciatic nerve pain in patients is frequently attributed to muscle strain or aging before imaging confirms a spinal source. When symptoms are consistent, persistent, or worsening, evaluation becomes the necessary next step.
Certain symptoms require more urgent attention. Loss of bladder or bowel control alongside lower extremity symptoms may indicate significant spinal cord involvement and should be evaluated promptly.
Treatment Options for Sciatica & Radiculopathy
Treatment is structured around the underlying cause, the severity of nerve involvement, and how long symptoms have been present. Most patients with sciatica or radiculopathy do not require surgery, though the appropriate path depends heavily on what imaging and evaluation reveal.
Conservative and Activity-Based Care
When symptoms are recent and nerve function remains intact, the first phase of treatment typically includes:
- Relative rest, activity modification, and avoidance of positions that increase nerve loading
- Physical therapy with a focus on nerve mobility, core stabilization, and posture correction
- Anti-inflammatory medication to reduce acute inflammation around the affected nerve root
- Structured monitoring to track symptom progression and identify whether the condition is resolving or advancing
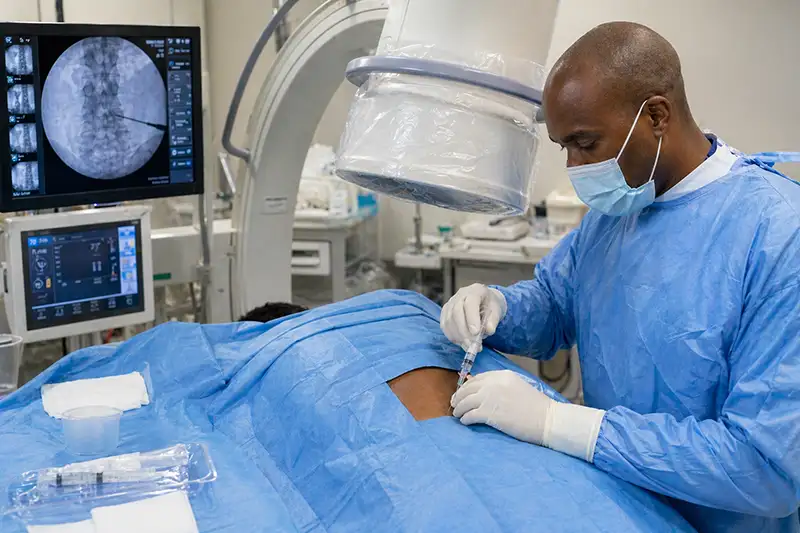
Interventional Pain Management
When symptoms do not improve with conservative care, or when nerve pain is significantly limiting daily function, targeted procedures can reduce inflammation directly around the compressed nerve and help restore mobility:
- Epidural steroid injections, which deliver anti-inflammatory medication into the epidural space surrounding the affected nerve root. These are among the most established approaches for managing lumbar radiculopathy when disc herniation or stenosis is the primary driver.
- Selective nerve root blocks, used both diagnostically to confirm which level is causing symptoms and therapeutically to reduce local inflammation.
- Facet joint injections, when facet-mediated inflammation is contributing to nerve irritation at a specific spinal level.
- Radiofrequency ablation, when pain is confirmed to originate from the facet joints and longer-term relief is needed.
Targeted Procedures
When a specific structural contributor is identified, additional options may be appropriate:
- Disc-focused interventional procedures, used when disc material is confirmed as the primary cause of nerve compression.
- The MILD procedure, considered when ligament thickening is contributing to canal narrowing and subsequent nerve irritation.
- Spinal cord stimulation, an option for patients with chronic radicular pain that has not responded to other treatments. SCS works by modifying how pain signals are processed before they reach the brain.
When Symptoms Continue or Worsen
If radiculopathy progresses despite conservative and interventional care, or when imaging identifies severe nerve compression, the evaluation moves toward surgical assessment:
- Advanced MRI review to confirm the level and extent of nerve root involvement
- Neurosurgical or spine surgery consultation when structural findings are significant
- Surgical decompression, such as discectomy or laminectomy, considered when nerve function is clearly at risk or conservative options have not provided adequate relief
The goal across all phases of sciatica treatment is to reduce pressure on the nerve, restore function, and prevent further structural progression. The right starting point depends on the findings at evaluation, not on a predetermined protocol.
Frequently Asked Questions About Sciatica & Radiculopathy
How do I know if my leg pain is sciatica?
The pattern is one of the clearest indicators. Sciatica typically produces pain, tingling, or numbness that starts in the lower back or buttock and travels down one leg, sometimes reaching the calf or foot. Pain that stays in the lower back without radiating into the leg is less likely to be sciatica. A clinical evaluation with imaging can confirm whether the pattern corresponds to sciatic nerve compression.
What is the difference between sciatica and radiculopathy?
Sciatica is a type of radiculopathy. Radiculopathy is the broader clinical term for symptoms caused by a compressed or irritated nerve root anywhere in the spine. Sciatica specifically refers to radiculopathy involving the sciatic nerve, which originates in the lumbar and sacral spine. When someone uses the term sciatica, they are describing a symptom pattern. Radiculopathy is the diagnosis that explains it.
Does sciatica go away on its own?
It can. When caused by a disc herniation, sciatica sometimes resolves over weeks to months as the disc material reabsorbs and inflammation decreases. However, not all cases follow this course. Symptoms that persist beyond six to eight weeks, worsen progressively, or involve weakness are generally not managed with a wait-and-see approach alone. Evaluation helps determine whether the underlying cause is likely to improve without intervention.
What makes sciatica worse?
Prolonged sitting, forward bending, coughing, and straining tend to increase pressure within the disc and along the nerve pathway, which is why many patients notice that sitting for extended periods is particularly uncomfortable. Positions that place the spine in flexion often provoke symptoms, while walking or lying flat may provide some relief, though this varies depending on the structural cause.
Can radiculopathy cause weakness, not just pain?
Yes, and weakness is often a more significant finding than pain. When nerve compression is severe enough to disrupt motor signals, the muscles supplied by that nerve can become weak or difficult to control. Foot drop, difficulty gripping objects, and muscle wasting are examples of motor involvement that require more careful attention and typically accelerate the timeline for evaluation and treatment.
Will I need surgery for sciatica treatment in NJ?
The majority of patients with sciatica or lumbar radiculopathy in NJ are managed without surgery. Surgery is considered when nerve compression is confirmed to be severe on imaging, when significant motor weakness is present, when bladder or bowel function is affected, or when symptoms have not improved despite a structured course of conservative and interventional treatment.
Is sciatica the same on both sides?
Typical sciatica affects one side. The nerve root compression responsible for sciatica usually occurs at a single level on one side of the spine, producing unilateral symptoms. Bilateral sciatica, where symptoms appear in both legs simultaneously, can occur but often suggests central canal narrowing rather than a single disc herniation. Bilateral symptoms warrant a more detailed evaluation to assess the extent of spinal involvement.
How long does nerve pain from radiculopathy last?
Duration varies considerably depending on the cause, severity, and treatment approach. Mild cases related to disc herniation may resolve within several weeks with appropriate care. More persistent cases, particularly those involving stenosis, bone spur formation, or longstanding compression, may require longer management timelines. Early evaluation helps establish a realistic expectation and the most effective treatment path.